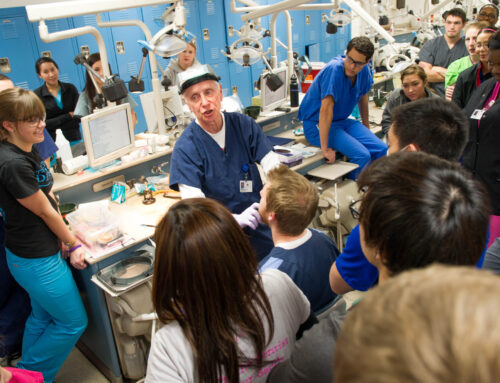
John Logan would like more than anything to keep up with his grandchildren: Photo by Danny Fulgencio
The day he started losing control of his body, John Logan was playing golf.
After a successful career as a pilot, he retired at 60 and played at least twice a week. The next five years were golden.
Cruising along a sunlit path one warm spring afternoon in 2005, he meant to slow and stop the golf cart.
His brain told his left foot to tap the break. His foot would not cooperate.
“My [reaction] was slow. And my foot shook.”
John remembers the cart fishtailing. Afterward he sat there, confused and frustrated.
“When this came up, well, it’s early spring, it’s 72 degrees, the trees are blooming,” he says, “And here I am trying to figure out this bad thing happening with my foot.”
By fall 2014, John Logan’s body was wracked by Parkinson’s disease. He had lost himself. His exceptional coordination, abundant golfing prowess, quick wit, life-of-the-party reputation and twinkling smile — all gone.
A relatively new technology called Deep Brain Stimulation, though complicated, risky and not entirely predictable, offered a chance to get it back. DBS involves brain surgery to implant electrodes in various areas of the brain and, after several weeks to heal, programming them to stimulate areas at the root of neurological problems.
On Oct. 9, John’s son Kevin recorded the dramatic post-operation session.
The video shows John entering the doctor’s office.
Tremors engulf his body — his legs, arms, trunk and head shake nonstop. He sits, and the doctor begins pressing buttons on a handheld control.
The video fades to black and resumes later that day, back at the Logan home.
John is sitting on the leather couch, utterly still. Off camera, Kevin says, “Dad, let’s go to the kitchen.”
[quote align=”right” color=”#000000″]“Kids, they can just accept things. ‘I have a granddad who falls down, a granddad who shakes real bad.’ They are like that.”[/quote]John stands and walks to the kitchen, unassisted.
Cynthia, John’s wife of 35 years, laughs, delighted.
“That has not happened in years,” Kevin says.
John turns to the camera, smiling broadly, and raises his arms, like Rocky, in sign of victory.
The graphics on the screen read, “Take that Parkinson’s.”
Kevin calls the DBS treatment a miracle.
“There is no such thing as a simple miracle,” warns the tagline of the 1990 movie “Awakenings,” which depicts the true story of Dr. Oliver Sacks, who treated a neurological illness called encephalitis lethargica that sends its victims into catatonic states.
With medication, Sacks brought his patients back to the world, but only temporarily.
The story forces its audience to consider complex questions such as, Is it better to remain hopeless or to be given hope and lose it?
Though not as extreme, John Logan and possibly other patients undergoing Deep Brain Stimulation share something like Dr. Sacks’ patients’ bittersweet experience.
John Logan does not feel as good as he did in Kevin’s video, and that, he says, is maddening.
After nine years of suffering, he had a day of normalcy before once again developing Parkinson’s symptoms. His condition is vastly improved — any observer can tell — but he is not satisfied.
“I want to feel the way I felt the first day,” he says. “Since then there has been a setback.”
In addition to presenting psychological ups and downs, Deep Brain Stimulation demands diligence, extensive testing and preparation, and maintenance that includes frequent follow-up visits. (In fact, the Logans moved to Lake Highlands partly to be close to their grandchildren but also to be close to Presbyterian Hospital.)
John bears the scars of holes drilled into his skull and a pacemaker-type neurotransmitter sewn into his chest.
But the many nuances of the technology also leave room for the family, all struggling with some feelings of disappointment, to hope.
Improvements are not necessarily immediate, programming occurs over a period of time, and it is not uncommon for patients to experience depression when results do not meet their expectations, according to Malcolm Stewart and Michael Desaloms, the neurologist and neurosurgeon, respectively, who treated John and wrote a paper about Deep Brain Stimulation in the Journal of Neuroscience Nursing.
“In general, frequent adjustments, one or two times a month for three months, are necessary to achieve good results,” the doctors write. “After three months the patient may come in for fine adjustments on an as-needed basis.”
Specialists also will tweak John’s medication until they find the optimal combination of electrical stimulation, medication and physical therapies — patience and persistence will be key for all involved.
Best-case scenario, the DBS treatment will help keep symptoms of Parkinson’s — including poor posture, speech impairment, gait freezing, balance problems and dementia — under control for years. Recent studies show symptom control beyond five years, but the outcome depends on myriad factors. “The success of this treatment, from patient selection to post surgery, is directly related to the expertise and collaborative endeavors of a team of medical professionals and support from the family and community,” John’s doctors note.
John officially was diagnosed with Parkinson’s, a progressive neurological disease that impairs movement and has no cure, in 2007, two years after his symptoms emerged.
“The first thing you feel is scared,” John says. His family — Cynthia, Kevin and his other son, Colby — shared his distress.
“You don’t see it all at once, but you gradually see little things deteriorate. It was hard for me to watch,” Kevin says. “When his brain is firing on all cylinders, my dad is the one who walks into the room and knows everyone within minutes. He leads every conversation. Always has a comeback.”
Cynthia, too, hated watching John, “the man of my dreams,” agonize.
When John was diagnosed, Cynthia was working some 60 hours a week as associate pastor at First Presbyterian Church.
“I was torn,” she says. “I loved work, but I wanted to be home with John. Before, I never worried, because he was on the golf course.”

Due to Parkinson’s symptoms, John Logan has not been able to golf, but Deep Brain Stimulation offers hope: Photo by Danny Fulgencio
Eventually John could not rise from a sitting position without help or walk without a cane. His tremors, fatigue and loss of balance caused him to fall more times than family members can remember.
He recalls a time he fell in front of his grandson, Kevin’s 3-year-old Finn. “He said, ‘Granddaddy, did you hurt?’ ” but after a little talk, John says, Finn was OK.
“Kids, they can just accept things. ‘I have a granddad who falls down, a granddad who shakes real bad.’ They are like that.”
John describes other frustrating misfires.
“I could have something in my mind to say, and by the time I turn to you to say it, it’s gone.”
He developed trouble keeping his eyes open, and his vision blurred. His muscles tensed, and his vocal chords weakened until his voice was a whisper.
He found some relief through the Parkinson Voice Project, a Far North Dallas-based nonprofit dedicated to helping people with Parkinson’s regain and maintain their voices.
“The voice was a big thing,” Cynthia says. “Everyone with Parkinson’s should know about the Voice Project.”
John scolds himself for not working enough lately with the voice project.
“I would be talking to you in a louder voice,” he says.
As the illness progressed, John all but stopped laughing or even smiling.
“That was probably the worst thing of all,” Cynthia says. “He developed what they called the mask face. John is personality plus, and his smile and warmth just radiate and he wasn’t able to express that — and that made me extremely sad.”
The first medicine prescribed to treat the tremors, Sinemet, nearly killed John.
It stopped his heart in the middle of a church program, Cynthia says.
“And that’s how we found out he was allergic.”
In December 2014, about two months after the programming, John Logan is on his feet. He answers the door of his Lake Highlands home and greets visitors with a firm “Hello” and a warm grin. The Logans are preparing to host a neighborhood holiday party, something Cynthia says would not have been possible pre-DBS.
Their miniature schnauzer, Sophie, is at John’s feet as he walks, no cane necessary, and she rests her head on his leg when he sits.
John is not cured. His right hand still bounces after he sits a while. His voice weakens in the course of conversation, and eventually he can’t entirely make his eyes stay open, though he is awake.
But when he does speak, he sometimes jokes, and when he hears something funny, he smiles, and if you are lucky, he laughs his famous belly laugh.
And in the last two-plus months, he has not taken a single tumble.
Cynthia came home the other day to see him sitting on the floor of their atrium with his grandson.
“The last time I found him on the floor, he had fallen,” she says. “This time he was playing with Finn.”
He even got up by himself, she adds.
And the other day when the grandchildren were visiting, they pulled an old putter from the garage.
“That day he swung a golf club — followed through and everything,” Cynthia says, “for the first time in years.”
As the family sits around discussing illness and mortality, among other things, it is clear they have not lost their sense of humor.
Cynthia mentions coolly that she has been diagnosed with Multiple Sclerosis, then she jokes that she and her husband are neurological wonders.
She has resigned from her post at First Presbyterian.
They talk about how John’s ocular tremors caused him to see moustaches on everyone on TV, even Angelina Jolie. John laughs louder than anyone at one point. Cynthia calls his expressiveness “magical.”
They also seem comfortable with serious feelings.
“He is a great friend,” Kevin says of his father. “He supports his friends and is there for them, and so they are there for him. And he’s a great dad.”
Cynthia’s eyes brim with tears when talking about the support they’ve received.
“I will say this, and I think he’ll agree, it was our family. Not just the boys, but the church family, neighbors, John’s brother, wife, cousins — he has more cousins than dogs have fleas — they all came forward. It was a strange time,” she says of the period leading up to John’s surgery. “I would not have made it without all those people.”
No one seems to have given up on further improvements, on getting John back to the day in the video.
“We have hope to get him where he wants to be,” Cynthia says.
“Maybe we can get him back on the golf course,” Kevin says. “Don’t you think, Dad?”
John’s eyes close — he is powerless to keep them open by now. But he answers, “Yes.”