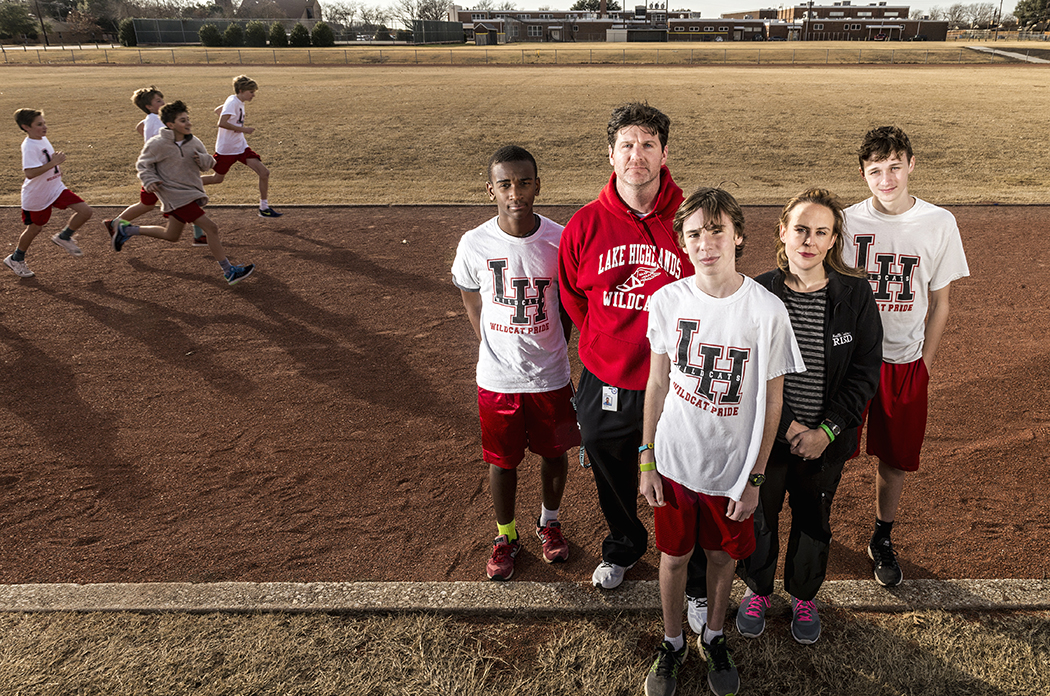
Blessed Divounguy, Craig Titsworth, Annie Young and Max Orvik surround Joe Krejci, whose life they teamed up to save. (Photo by Danny Fulgencio)
A relatively modern medical device — and staff who appreciate its importance — is saving lives at neighborhood schools
In racing, every second counts. It was especially true one afternoon last December at Lake Highlands Junior High, when track coach Craig Titsworth assigned his sixth-period runners a relatively benign offseason workout — a few 100-, 200- and 400-meter intervals.
As the first group barreled toward its destination, 13-year-old Joe Krejci hit the ground.
It’s an old cinder track, so trips and falls are not uncommon, the coach explains, and for a second, no one thought much about it. But then Joe didn’t get up.
“Coach T” was some 90 meters away from the incident, he says, when he saw concerned looks cross the other boys’ faces, and they motioned for him to come.
“I sprinted, and I saw him, unconscious. I called 911.”
Titsworth handed the phone to a student, who briefed the operator, as the coach sprung into action.
“I checked his head, stabilized his neck, felt for bumps or blood …”
He had a slight pulse, but he was not breathing.
“I looked up to see the two fastest kids in the district standing over me,” Titsworth says. “I mean, I’m thinking, God’s provision, right? These guys, Max Orvik and Blessed Divounguy, are not just our two fastest eighth-graders — they were first and second in the last citywide track meet — these are the fastest [middle school] runners in all of Richardson ISD.”
Find the school nurse, Coach T told them. They tore toward the building — which sits several hundred yards from the track, the nurse’s office at the opposite end — while the coach debated whether to start CPR. Trained in first-aid, he knew he was not supposed to if the patient was breathing. But was this breathing? Still unconscious, Joe imparted these strange deep shaky gasps.
“I later learned this was agonal respiration, death breath, and he wasn’t actually breathing, not really. His pulse was what my EMT [emergency medical technician] brother would call thready, he was turning blue, and drawing these labored breaths every 15-20 seconds.”
Then the runners were back. Alongside them hurried an out-of-breath nurse Annie Young, carrying an A.E.D., an automated external defibrillator designed to shock an arresting heart back into rhythm.
In 2007, Texas passed a law requiring an A.E.D. in every Texas school.
“Something just told me to grab it,” Young says. “It was the looks on the boys’ faces and the way they said ‘collapsed’.”
The team, Young, front office administrator Syreeta Love and God, all are to thank for Joe’s survival, Titsworth says. But if not for that small piece of medical technology, which staffers at every Richardson ISD campus are trained to use, he knows things could have been devastatingly different.
The coach hurdled the chain-link fence surrounding the track, grabbed the A.E.D., leapt back over and put the pads on Joe’s chest and left side.
The device registers, checks for an unsynchronized heart rhythm (the cause of most sudden cardiac arrests, according to the American Red Cross) and displays instructions.
“Shock advised,” it read. So Coach pressed the machine’s “shock” button, delivering an electric volt through Joe’s chest to his heart.
By then Love and Young were assisting, the nurse administering chest compressions.
The track coach, by profession a stickler for time, notes that Joe dropped to the ground at 3:04 p.m. He delivered the shock at 3:12 p.m. The ambulance arrived at 3:15 p.m.
As the ambulance pulled away, the coach and the boys who ran for help all worried that they hadn’t acted fast enough, they all say days later.
“I wondered, what if I didn’t run fast enough,” Max says.
At the hospital that night, while Titsworth visited, doctors told Joe and his parents that the shock saved him — that he could have died if they’d waited even a couple more minutes.
In fact, a victim’s chance of surviving this type of cardiac arrest “drops by 10 percent for every minute a normal heartbeat is not restored,” according to the American Heart Association.
Doctors outfitted Joe with a pacemaker, the teen was back at school before Christmas break.
“I don’t remember anything, really,” Joe says. His friends filled him in when he returned to school.
Coach Titsworth, nurse Young and administrator Love are part of their school’s emergency response team. At every Richardson ISD campus, teams of five-to-10 staffers, usually front office personnel and coaches, are specifically trained for critical situations, explains Richardson ISD special assignments nurse Alicia Whitehead, who has coordinated CPR and first aid training for district employees for 11 years.
“We take it very seriously,” she says of the emergency response program, “because we want our students to be safe.”
When the A.E.D. rule went into effect, it wasn’t easy to implement.
“They made the law, but did not provide the funds,” she says. She points to one model that costs about $1,400, explaining that price varies for sizes (the A.E.D.s in

The emergency response team at Wallace Elementary — including Kendra Smith Worthey, Shannon Young Domizio, Lauren Bolack, Audrey Clary and Jessica Haas — surround cardiac arrrest victim Sarah Maupin. (Photo by Danny Fulgencio)
elementary schools are smaller, for example).
Still, the district allocates money not only to place and maintain the requisite A.E.D.s in every school (five high schools, eight middle schools and 41 elementary schools) but also to add multiple devices in the bigger campuses and even more at the high schools.
In district sports, team managers carry portable A.E.D.s. Choir and band directors carry them when the groups travel.
“We are required by law to check each once a month, but we check them daily,” Whitehead says.
The devices are stored in recessed, reachable cabinets, usually in school hallways, outside a nurse station or the gym. Bright, visible signs, posted around campuses, advertise A.E.D. locations.
Though several employees at each school are trained to use an A.E.D., the machine is user friendly even for a layperson in an emergency.
“It talks to you. It tells you what to do,” Whitehead says. “We want them to be accessible, even if it’s at an event after hours and the nurse is not around.”
Considering that sudden cardiac arrest is by far the leading cause of death in student athletes, one would think every school in the nation would take A.E.D.s and training as seriously as RISD.
But that isn’t the case, according to an article last April in the New York Times:
“Many [A.E.D.s] are locked up in an office and not accessible, or only the school nurse knows how to use it,” Fort Worth mom Laura Friend tells the paper. Friend lobbied for the A.E.D. law after losing her daughter to cardiac arrest in 2004, and she created a nonprofit that has donated A.E.D.s and provided training throughout Texas.
Dr. Jonathan Drezner, director of the Center for Sports Cardiology at the University of Washington, told the Times that, “During the academic school year 2014-15, there were 55 cases of cardiac arrest among [student athletes], and 57 percent died. I can’t believe we don’t have universal access to A.E.D.s in schools; they should be like fire extinguishers.”
The decision to invest in A.E.D.s and training several years ago was good planning, says RISD communications director Tim Clark.
A.E.D.s have been used as an emergency response on at least five occasions that he can recall. And most importantly, “we have never lost anyone as a result of cardiac arrest, at least in the 15 years I have been around.”
Nurse Whitehead recalls that two years ago in February, “I remember because it was American Heart Month, a trainer with a portable A.E.D. saved a Richardson High School football player who collapsed after practice.”
Remarkably, it was just two weeks prior to Joe Krejci’s near-death experience that an equally dramatic incident unfolded at Wallace Elementary, less than a half-mile away from the LHJH track.
Wallace’s nurse, Jessica Haas, who also is a parent, was leaving a parent-teacher meeting when her husband saw a woman collapse on the sidewalk in front of the school.
“He knew right away that it was something bad,” Haas says, “because he saw her go right down, didn’t try to catch herself or anything.”
The woman, Sarah Maupin, who also was leaving conference with a teacher, had suffered a cardiac arrest.
Haas rushed to help Maupin, who was unresponsive and without a detectable pulse.
Even though it was late, five members of Wallace’s emergency response team — executive assistant Shannon Young Domizio, assistant principals Lauren Bolack and Kendra Smith-Worthey, Audrey Clary and Haas — for various reasons happened to be at the school.
“Therein lies the miracle,” Haas says.
Haas instructed the nearest of them to grab the A.E.D.
Within minutes Haas was delivering a salvaging shock to Maupin’s heart.
Though Maupin doesn’t remember it, thanks to the device and the well-trained responders, she had regained her steady heartbeat and consciousness before the ambulance arrived.
Maupin’s doctor told her how rare it was for someone in her situation to receive such quick and apt attention, and how lucky that made her.
“The results could have been detrimental,” Maupin says. “After 4 minutes [of unconsciousness following an attack] you can have brain damage. It could have been that, or even worse.”
Nurse Haas says she heard activist Laura Friend’s story a few years ago during a district first-aid training workshop.
“Her daughter died at a swimming pool, where there was an A.E.D. but no one knew about it or knew what to do,” she recalls. “We’ve all heard these accounts of people collapsing and dying even though an A.E.D. is on site.”
That nothing like that ever happens at an RISD property or event, she and her team members agree, is the goal.
President Lyndon B. Johnson declared the first American Heart Month in 1964. Ever since then, the month of February has been dedicated to cardiovascular health. Learn more about Heart Month, related events, local CPR classes and A.E.D.s at heart.org.